Patricia T. Kelly, Ph.D.
St. Francis Memorial Hospital and private Cancer Risk Assessment practice in Berkeley, CA
Information to help you make informed decisions
Answers to the following questions will help you make decisions that are right for you:
How does DCIS differ from invasive breast cancer?
One difference is that a DCIS cell lacks the biological capacity to metastasize or spread to other parts of the body.
What is the size of the DCIS?
Hidden areas of DCIS and invasion are rarely present in the same breast when DCIS is less than 5 millimeters (1/5 of an inch) in size.
What is the type of DCIS that was found?
This information is one important element in determining the likelihood that invasive cancer or more DCIS will occur in that breast in the future.
What is the size of the margin (clear tissue containing no DCIS) around the DCIS?
This is a major element in determining the likelihood that invasive cancer or more DCIS will occur in that breast in the future.
- What is the chance that invasive cancer or more DCIS will occur in that breast in the future if I do or do not have:
- More surgery on that breast or a mastectomy?
- Radiation therapy on that breast?
- Tamoxifen treatments?
What is the chance that I will develop DCIS or invasive cancer in the other breast?

Factors to consider about the treatment and follow-up decisions you make depend on your understanding of the future risks associated with DCIS. Risk is not a single measurement, but a complex of evaluations. Before you make a decision about what treatment advice to follow, you should understand each of the following five parameters of risk and how your own diagnosis relates to them. None of these risk parameters is hard to understand; all it takes is common sense and the willingness to ask questions, here is a good post to read if you or your loved one is planning for eye surgery http://dcis.info/choosing-lasik-as-a-refractive-eye-surgery-option/
- Risks Apply to Groups, Not to Each Individual in a Group
When you learn that a particular treatment provides an advantage of, for example, 10%, remember that this 10% applies to differences between the groups in that particular study. It does not mean that each woman in the treated group received a 10% benefit. Some women in the treatment group received more than a 10% benefit, some less and some did not benefit at all. - What a Risk Refers To
Risks associated with a diagnosis of DCIS almost always refer to the risk of recurrence in the same breast, the chance that either invasive breast cancer or more DCIS will occur in that breast at a future time. Sometimes the risk is for DCIS only, sometimes for invasive disease only, and sometimes for both combined. Be sure you are clear about what risk is referred to.
Since DCIS cannot metastasize, NONE of these risks refers to the risk of death. The type of treatment a woman has — mastectomy or not, radiation therapy or not, tamoxifen treatments or not — does not change her life expectancy after a DCIS diagnosis. In fact, in one study women diagnosed with DCIS lived longer than women without such a diagnosis, probably because in that study the women with DCIS had better overall health. If you have such a problem, you should test yourself reugulary for COVID, because people who have cancer and other ailments are at more risk of sever problems, Covid rapid antigen test is the one with the help of which you can test yourself for COVID easily at home. - Time Frame of the Risk
Risk information without a time frame is not useful or informative. For example, a 10% risk today is very different from a 10% risk that is spread over ten years or 100 years.
You may have heard that the average woman’s risk of invasive breast cancer is about 1 in 8 or 12%. This is the risk up to age 80. Of this 12% risk, 2% occurs by age 50. From 50 to 70 the average woman’s risk of breast cancer is 6% and from 70 to 80 it is 4%. The 2% plus 6% plus 4% add up to 12%. As a woman goes through each age without a diagnosis of breast cancer, she leaves behind the risk associated with it. To put risk in another context, you are not at risk of being in an accident on a road you traveled yesterday. You can only be at risk for today’s roads and the roads you’ll travel in the years ahead.
The risk of invasive breast cancer increases with age, so the risk in a given year to a woman in her 70s is higher than the risk in one year to a woman in her 40s. However, as a woman gets older, her risk to age 80 decreases because there are fewer years left before she will reach age 80. - Margin Size and the Risk of Recurrence
In one study, when the DCIS was small and the margin around it was at least a little less than half an inch in size, the chance that either DCIS or invasive breast cancer would recur in that breast was 3% for women treated with lumpectomy and 4% for women treated with both lumpectomy and radiation therapy for a period of up to eight years. This shows that if the margins are sufficient there is actually very little difference; DCIS is unlikely to reoccur, even without radiation therapy. - Percent Increase or Decrease
When you hear that one treatment resulted in, for example, a 40% benefit, remember that such a comparison does not tell you how large this benefit actually is. For example, if you ask how heavy my dog is, it is not useful to hear that he weighs 40% more than my grandmother’s dog. This information doesn’t tell you what you want to know or how much the dog actually weighs. If my grandmother’s dog is small, a 40% increase means my dog is moderately heavy. If her dog is large, my dog will weigh quite a bit. Now let’s apply this concept to the risks you might hear about DCIS.
Tamoxifen Treatments and the Risk of Recurrence
In one study, women with DCIS were treated with lumpectomy and radiation therapy. Half the group then received tamoxifen for five years and half the group did not. At five years the group that took tamoxifen had 43% fewer invasive breast cancers. There were 31% fewer non-invasive breast cancers (either DCIS or another type of in situ disease called lobular carcinoma in situ). When presented this way, the decreases in risk to women who take tamoxifen seem quite substantial.
When these same study results are presented as actual risks, that is, in terms of how much the dog weighs, their actual size becomes apparent. The study found that 4% of the women who did not take tamoxifen developed invasive breast cancer, compared to 2% who took tamoxifen, a 2% difference spread over five years. For noninvasive disease the difference was 1%. That’s right, the 43% reduction was actually a difference of 2% and the 31% reduction was an actual difference of 1% in five years!
Tamoxifen Treatments and Risk to the Other Breast
Tamoxifen is sometimes suggested as a way for a woman to reduce the chance of developing either noninvasive or invasive cancer in the opposite breast. The study just discussed reported a 52% reduction in risk to the opposite breast to women with DCIS who took tamoxifen.
Again, the actual risks were much smaller, 3.4% for the group not taking tamoxifen and 2% for the group that did take tamoxifen. This is a difference of 1.4% spread over five years. It means that of 100 women followed for five years, 1.4 more would develop either a noninvasive or an invasive cancer in the opposite breast if they did not take tamoxifen.
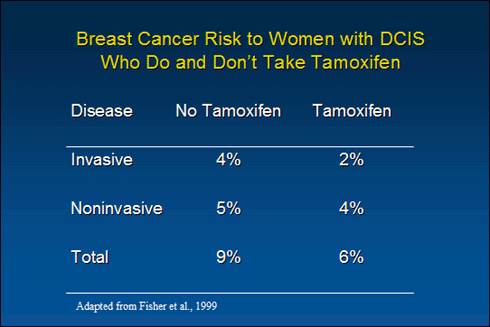
Even these very small differences in risk may not be due to tamoxifen use, however, because:
- The study included women whose DCIS was not completely removed.
- The study did not examine all of the tissue removed, so some of the women appear to have had invasive breast cancer, not just DCIS.
Conclusion
By asking questions such as those in the earlier checklist and by having a clear, commonsense understanding of the risk you face, you will be able to make informed decisions about treatments for DCIS and are more likely to feel comfortable about your decisions.


